By Thabisani Dube
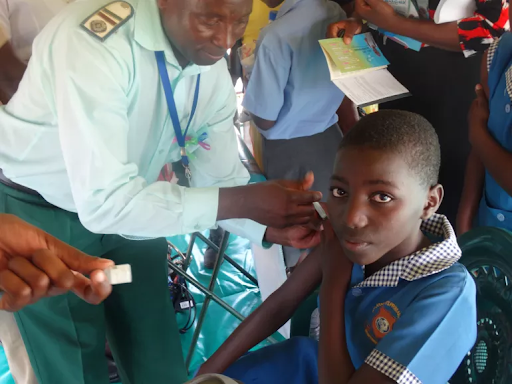
As the early sunlight shines over the dusty playground at Detema Secondary School in Matabeleland North, 11-year-old Kudzai Ndlovu hesitates just before entering her class. Nurses’ inside are preparing vaccines, while students from other classes discuss this day’s activities in hushed tones. After Kudzai takes a deep breath, she goes into her classroom.
In 2018, Zimbabwe introduced a national Human Papilloma Virus (HPV) vaccination programme targeted at girls aged 10-14. This initiative provides protection to these young women from the two main types of viruses that cause most of all cervical cancers. In total, there were around 3000 new cervical cancer diagnoses per year, resulting in over 2000 annual deaths, according to the World Health Organisation (WHO). The goal of the project – backed by UNICEF, WHO and GAVI-The Vaccine Alliance – is to administer vaccinations to young women prior to their being exposed to the viruses and reduce the long-term emotional and economic burdens placed upon both the families and the healthcare delivery systems.
“I was scared,” said Kudzai quietly after receiving her vaccination. It is common across Zimbabwe for individuals to practice fear associated with injections, rumours concerning potential negative reactions caused by the vaccine and concerns within some religions, such as the Johane Marange Apostolic Church, regarding the use of vaccinations.
At Detema, Deputy Head of School Siphilile Mkosana stated that the school provides awareness education prior to immunisation days.
“Schools teach pupils about HPV and the significance of the vaccination,” she said. “However, some parents withdraw their children from school due to misconceptions or fears related to vaccinations.”
Nurse Nozihlobo Ncube, who works as part of a district nursing team providing support for outreach programmes within schools located in Tsholotsho District, in Matabeleland North province indicated that early involvement in schools and families has resulted in a number of positive outcomes.
“We meet with both teachers and parents prior to administering the vaccine,” she said. “When we educate our community about the vaccine, they can be less resistant to accepting it.”
The vaccine used in Zimbabwe protects against HPV strains 16 and 18, which cause the majority of cervical cancer cases. Globally, cervical cancer kills more than 300,000 women each year, with 85 per cent of cases occurring in low- and middle-income countries, says WHO.
Despite its effectiveness, uptake in Zimbabwe is uneven. Murewa, Makoni and Tsholotsho achieved 75–86 per cent full coverage through school campaigns (2019 national survey), though some areas dipped below 70 per cent due to misinformation and logistics. Health workers say clear communication, local trust-building and routine school outreach are key to closing those gaps.
Not all parents are convinced. In Harare, mother of two Charity Mudavanhu says she stopped her other daughter’s vaccination after the first girl began menstruating earlier than expected following an injection. Clinical trials and ongoing monitoring show the vaccine is safe; common reactions are usually mild arm pain or a slight fever.
“I became afraid and decided not to continue,” she says. Health authorities, however, note there is no scientific evidence linking HPV vaccination to early menstruation.
For other parents, understanding changes everything. “I was unsure at first,” says Loretta Ncube, a parent in Gweru, Midlands Province. “But after the nurses explained, I agreed because it protects her future.”
Apprehension eased across sites.
“It was quick,” Kudzai added after her injection. In Mvurwi in Mazowe District in Mashonaland Central, 12‑year‑old Tafadzwa Chikowero said: “I’m happy I did it.” In Harare, a quieter relief was common among pupils who had been nervous beforehand.
Lovemore Makurirofa, Advocacy and Communications Officer at the Cancer Association of Zimbabwe (CAZ), calls the vaccine a critical long-term intervention.
“Although its impact is long-term, it significantly reduces the risk of young girls developing cervical cancer later in life,” he says, noting that prevention is more sustainable than the costly treatments many communities cannot access.
Makurirofa emphasises that in a resource-constrained environment, the vaccine is a mechanical necessity.
“In a developing country like ours, where resources are very limited, we need to focus more on the prevention,” he says. “The HPV vaccine is one of the very important cervical cancer prevention interventions.”
He warns, however, that the shadow of previous health crises lingers over the programme.
“The same misinformation we saw during the COVID-19 period is common in our communities,” Makurirofa explains, noting that it is the responsibility of both the Ministry of Health and Child Care and civil society to “disseminate correct information to convince the communities that it has been piloted and considered safe.”
Public health experts stress that up to 90 per cent of cervical cancer cases are preventable through vaccination, screening and early treatment. Yet screening rates in some parts of Zimbabwe remain below 20 per cent, making vaccination an especially important tool now.
Beyond individual protection, the programme aims to ease future pressure on health services by reducing demand for chemotherapy and radiotherapy, and to advance equity by reaching rural learners through school-based delivery. UNICEF and WHO continue to support community engagement, while teachers, nurses and local leaders play central roles in addressing myths and cultural concerns. Studies on behavioural and social drivers of health show that trust and clear communication are key to improving uptake.
Regionally, countries such as South Africa, Zambia and Malawi face similar challenges: uneven coverage driven by misinformation, supply gaps and rural access barriers, despite ongoing HPV programmes. The World Health Organisation’s global strategy seeks to eliminate cervical cancer as a public health problem by 2030, targeting 90 per cent vaccination coverage, 70 per cent screening and 90 per cent treatment.
At Detema, as nurses drive away and dust settles, the playground returns to normal—but Kudzai and her classmates carry invisible protection. Caroline Mandishona from Budiriro, in Harare speaks for many parents: “We may not see the benefits now, but we know it protects her future.” Across Zimbabwe, one jab at a time, girls are gaining healthier tomorrows.